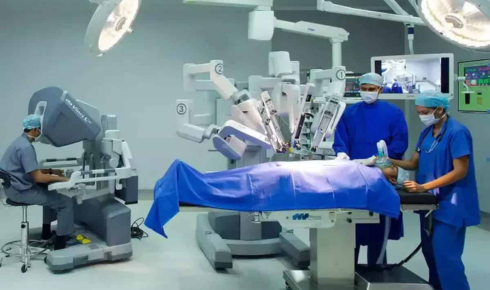
There was a time—not too long ago—when surgery felt like something distant, almost intimidating. White lights, steel instruments, the quiet tension in operating rooms. But today, something subtle yet powerful is changing that picture. It’s not just about machines or innovation for the sake of it; it’s about how technology is gently reshaping the way doctors care for people, especially in delicate areas like gastrointestinal health.
If you’ve ever had even a minor digestive issue, you’ll know how disruptive it can feel. Now imagine dealing with something more serious—ulcers, tumors, or chronic conditions that require surgical intervention. The good news? The approach to treating these problems is evolving, and in many ways, becoming more precise, more thoughtful… almost more human.
A New Era of Surgical Thinking
What’s interesting about modern medicine isn’t just the tools—it’s the mindset. Surgeons today aren’t just trained to “fix” problems. They’re taught to minimize disruption, preserve function, and think long-term. That’s where robotic surgical methods come into play.
Now, before it sounds too sci-fi, let’s clear something up. These systems don’t replace surgeons—they enhance them. Think of it like giving a skilled artist a finer brush. The control is still human, but the precision? That gets a serious upgrade.
With robotic-assisted systems, surgeons can operate through tiny incisions, using instruments that mimic hand movements but with greater stability. There’s less shaking, more accuracy, and a level of detail that wasn’t always possible before. It’s not about removing the human element—it’s about amplifying it.
Why Precision Matters More Than Ever
When it comes to gastrointestinal procedures, precision isn’t just a bonus—it’s everything. The digestive system is complex, tightly packed, and incredibly sensitive. A slight miscalculation can affect surrounding tissues, leading to complications or longer recovery times.
That’s why the concept of precision GI care has become such a cornerstone in modern treatment approaches. It’s not just about performing surgery—it’s about doing it in a way that respects the body’s natural structure and function.
Imagine a surgeon working on the colon or stomach with enhanced 3D visualization, able to zoom in and see layers of tissue more clearly than ever before. That level of clarity allows for better decision-making in real time. And honestly, that’s where outcomes start to shift.
Patients often experience less blood loss, fewer complications, and quicker recovery periods. It’s not magic—it’s careful, deliberate improvement in how procedures are performed.
The Patient Experience Is Changing Too
Let’s talk about something that doesn’t always get enough attention: how patients feel before and after surgery.
For many people, the fear of surgery isn’t just about the procedure—it’s about the unknown. Will it hurt? How long will recovery take? Will life go back to normal?
With newer surgical approaches, including robotic assistance, those questions are starting to get better answers. Smaller incisions often mean less pain. Shorter hospital stays mean less disruption to daily life. And in some cases, patients are back on their feet much sooner than expected.
It’s not perfect, of course. No medical procedure is without risks. But the direction is encouraging. There’s a growing sense that surgery doesn’t have to feel like a last resort—it can be a carefully managed step toward healing.
Behind the Scenes: The Surgeon’s Perspective
It’s easy to focus on the technology, but what about the people using it?
Surgeons who adopt these advanced systems often talk about the learning curve. It’s not just plug-and-play. There’s training involved, adaptation, even a bit of humility. After all, even experienced professionals have to rethink how they approach familiar procedures.
But once they get comfortable, many describe a noticeable difference. Better ergonomics, reduced fatigue during long operations, and a clearer view of the surgical field. All of this contributes to what ultimately matters most—improved outcomes for patients.
And maybe that’s the quiet beauty of it. The technology doesn’t shout. It doesn’t demand attention. It just works in the background, supporting better decisions, steadier hands, and more thoughtful care.
Not Just for Complex Cases
One common misconception is that robotic-assisted surgery is only for the most complicated conditions. While it’s certainly valuable in those scenarios, its use is expanding into more routine procedures as well.
From hernia repairs to certain types of bowel surgeries, the benefits of enhanced precision and control are being recognized across a broader range of treatments. It’s not about reserving innovation for rare cases—it’s about making everyday care better.
And that shift matters. Because most patients aren’t dealing with rare conditions—they’re dealing with common, often frustrating health issues that deserve just as much attention and care.
A Balance Between Innovation and Trust
Of course, with any new technology, there’s always a question of trust. Patients want to know: Is this safe? Is it proven? Is it right for me?
These are fair questions—and important ones. The reality is that robotic-assisted surgery has been studied extensively, with many procedures showing strong safety profiles and positive patient outcomes. But like any medical decision, it’s not one-size-fits-all.
What matters most is the conversation between patient and doctor. Understanding the options, weighing the benefits and risks, and choosing a path that feels right. Technology can guide the process, but it doesn’t replace that human connection.
Looking Ahead, Without Losing Sight
As we look to the future of surgery, it’s tempting to imagine even more advanced systems—AI integration, smarter diagnostics, maybe even fully automated procedures. But perhaps the real goal isn’t to remove humans from the equation.
Maybe it’s about making human care better.
Because at the end of the day, surgery isn’t just about fixing what’s broken. It’s about restoring quality of life, easing discomfort, and giving people a chance to move forward without pain holding them back.
And if technology—quietly, steadily—can help make that happen with more precision, less trauma, and greater confidence… well, that’s not just progress. That’s something worth paying attention to.